PARTNER CONTENT
Managing Diabetes
A. Living with Diabetes
Nicole Pelcz was diagnosed with type 1 diabetes when she was a teenager. “I have lived with diabetes for almost half my life.” She works for a charitable organization in Ontario managing healthy living programs.
“Living with type 1 diabetes is a 24/7 job. I have to think about diabetes all the time. It’s not something I can take a vacation from, opposed to most people who can walk away from their job for a weekend getaway,” explains Pelcz. “Diabetes impacts everything I do, this is why a positive outlook is vital,” she says. “I have to think about diabetes before I go to sleep, to make sure my blood sugars are in range when I’m sleeping, and just as I wake up before I even head off to work. I have to consider what I’m eating, because different foods affect my body and blood sugars differently. I have to think if I’m able to exercise at the time I want to, or sometimes I even have to wait to drive because a low blood glucose level can impact thinking, alertness and cognition.”
“Living with type 1 diabetes is a 24/7 job. I have to think about diabetes all the time. It’s not something I can take a vacation from.”
– Nicole Pelcz
B. Caregiver Challenges
Being a working parent caring for a child with type 1 diabetes can be challenging. Cyndi Orth works for a school district in Abbotsford, BC, and is a caregiver for her daughter Sophia who lives with type 1 diabetes. Sophia was diagnosed at three years of age and is now 18 and off to university. “When Sophia was young, I didn’t have any support for her in school and I had no family that lived close by. I had to go give her insulin injections at school. At that time, I was very fortunate and had an amazing boss. If I got an emergency call or text from the school that Sophia was running low, he would just say ‘go.’”
Sophia was hospitalized with diabetic ketoacidosis three times during her primary school years. When she was in hospital, Orth says, “I used up my sick days to be there with her. Fortunately, I had the flexibility to use them in that way and was never sick during her younger years.” When she ran out of sick days, Orth had to take days off without pay.
When Sophia was younger, either Orth or her husband would wake every day between 1:00 a.m. and 2:00 a.m. to check her blood sugar. “We were tired because of our interrupted sleep, which, of course, impacted our performance at work,” says Orth. “You try to get used to it, but you don’t, because sleep is important.”
Sophia is always top of mind for Orth and her husband. When Sophia was younger, they asked themselves, “How do we work today knowing that she is safe?” “We always arranged our schedule so one of us would be able to get to the school and look after her. I always had to have my phone on standby and close to me.”
Sometimes when Orth was presenting at work, she’d get a text or phone call. “I’d think, Sophia might be experiencing a low. Do I take it, or do I continue?”
When Orth knew that she wouldn’t be able to take a call, her husband, who used to be a travelling salesperson, arranged his schedule so he would be in the community that day in case Sophia needed help at school.
C. Diabetes Management
People living with diabetes must manage their blood sugar levels through lifestyle choices, diabetes technology and medication. The objective is to avoid life-threatening hypoglycemia (low blood sugar) and the potential of long-term damage of hyperglycemia (high blood sugar).44, 45
Diabetes management includes:46, 47, 48
- A healthy eating plan
- Physical activity
- Taking medicines that doctors prescribe to manage blood sugar, blood pressure, cholesterol levels
- Losing weight, if a person has overweight or obesity
Diabetes Canada ABCDES of Diabetes Care50, 51
A A1C targets
B Blood pressure (BP) targets
C Cholesterol targets
D Drugs for decreasing heart disease risk
E Exercise goals and healthy eating
S Screening for complications
S Smoking cessation
S Self-management, stress, other barriers
D. Diabetes Care – A Team Effort
“Diabetes support takes a healthcare team,” explains Quiambao. This may include family doctors, endocrinologists, nurses, dietitians, chiropodists, mental- health practitioners and pharmacists, along with social support from family and caregivers. “Coordinated care may be required because healthcare providers often work in silos, which can be challenging for people living with diabetes,” she says.
E. Diabetes Educators
Diabetes educators are a key member of the diabetes care team. They are health professionals who specialize in diabetes treatment who partner with people with diabetes and their families to teach, coach and guide them to develop behaviour-change goals to improve their health and to develop a management plan that fits their lifestyle, beliefs and culture.
“The approach of diabetes educators has been changing,” says Ontario-based Certified Diabetes Educator and Registered Nurse Connie Tanner. In the past, a diabetes educator would tell the person with diabetes what they needed to do and expect them to follow the instructions, she says. “Our role now is to provide the person with diabetes with the skills and knowledge they need to manage their condition, to help access resources they need, and support behaviour change and empowerment. In essence, we help the person with diabetes to identify what is important to them and support them in working toward their priorities.”
F. Whole Person Model for Holistic Care52
To deliver a better experience and generate positive outcomes, diabetes care should consider the whole person and look beyond simply their medical condition(s). Although a medical prognosis may be the same for two people, the best sup-port could be vastly different for each of them. Knowing the whole person allows their care plan to be tailored to the individual, and results in better outcomes.
“Our experience demonstrates that people living with diabetes have a higher incidence of being treated for heart disease, gastrointestinal issues and mental-health issues,” says Colleen Adams, manager, health & digital product solutions, Medavie Blue Cross. “This demonstrates the need to treat people living with diabetes holistically, with solutions that address more than just monitoring blood sugar levels.”
G. Glucose Levels53, 54, 55
Checking blood glucose levels is important for people with diabetes because the results help guide decisions about what to eat, physical activity and medication use to ensure that blood sugar levels are stable and in the healthy range.
There are over 40 factors that affect glucose levels, many of which are impossible to manage, remember or even account for, and not every individual will respond in the same way. The best way for people with diabetes to determine their impact is by monitoring their glucose and looking for patterns.56
Extreme blood sugar highs and lows can lead to major problems:
- Hypoglycemia (low blood sugar) can happen quickly and is important to treat right away. It can cause confusion and disorientation, or be more severe and cause loss of consciousness, seizure or coma.57, 58
Fear of hypoglycemia is when some people living with diabetes keep their blood glucose high to avoid severe hypoglycemia. This may lead them to make poor diabetes-management decisions, which can be a barrier to achieving their target glucose levels and lead to increased risk of diabetes complications.59
Hypoglycemia unawareness (or impaired hypoglycemia awareness) is when a person with diabetes doesn’t notice they have low blood sugar, as they do not experience usual early warning symptoms. Without warning, they lapse into severe hypoglycemia and may become confused or disoriented, experience convulsions or, in rare cases, fall into a coma.60, 61
- Hyperglycemia (high blood sugar) can cause long-term health complications caused by damage to blood vessels and nerves such as heart disease, kidney failure, stroke, heart attack, blindness and lower limb amputation as well as diabetic ketoacidosis, which is a poten-tially life-threating buildup of acids in the blood.62, 63
i. Monitoring Glucose Levels
There are a variety of ways to monitor glucose levels64, 65, 66
Capillary blood glucose meter (formerly known as blood glucose meter) uses a finger prick to check blood glucose levels.67
Intermittently scanned continuous glucose monitoring (isCGM) (formerly known as flash glucose monitoring) measures interstitial fluid glucose levels* with a hand-held scanner swiped over the sensor. Some systems are equipped with optional alarms to alert for low and high blood sugar.
Real-time continuous glucose monitoring (rtCGM) (formerly known as continuous glucose monitoring or CGM) also checks interstitial fluid glucose levels*; however, it provides a continuous display of blood sugar and uses an alarm to alert for low and high blood sugar.
A1C, also known as HbA1c, is a laboratory blood test that measures average blood sugar over the past three months.

*Works via a small sensor that is inserted just under skin that reads the glucose level in the surrounding interstitial fluid, which is a thin layer of fluid that surrounds the body’s cells.
Glucose Targets
According to Diabetes Canada, the recommended glucose targets for most people with diabetes are listed below, but they may be individualized based on discussions between a person with diabetes and their healthcare team. Diabetes Canada43 believes that people living with diabetes deserve to be spoken with and about in ways that are respectful, inclusive and value based, and recommend language used:
|
Targets for most people with diabetes68, 69 |
|
|
A1C |
7.0% or less |
|
Fasting blood glucose (sugar) – blood sugar before eating |
4.0 to 7.0 mmol/L |
|
Blood sugar two hours after eating |
5.0 to 10.0 mmol/L (5.0 to 8.0 mmol/L if A1C targets not being met) |
|
Time in Range (TIR) – % of time that person’s blood glucose level is in their recommended target range |
% of values between 3.9–10.0 mmol/L >70% |
ii. Time in Range70, 71, 72, 73, 74, 75
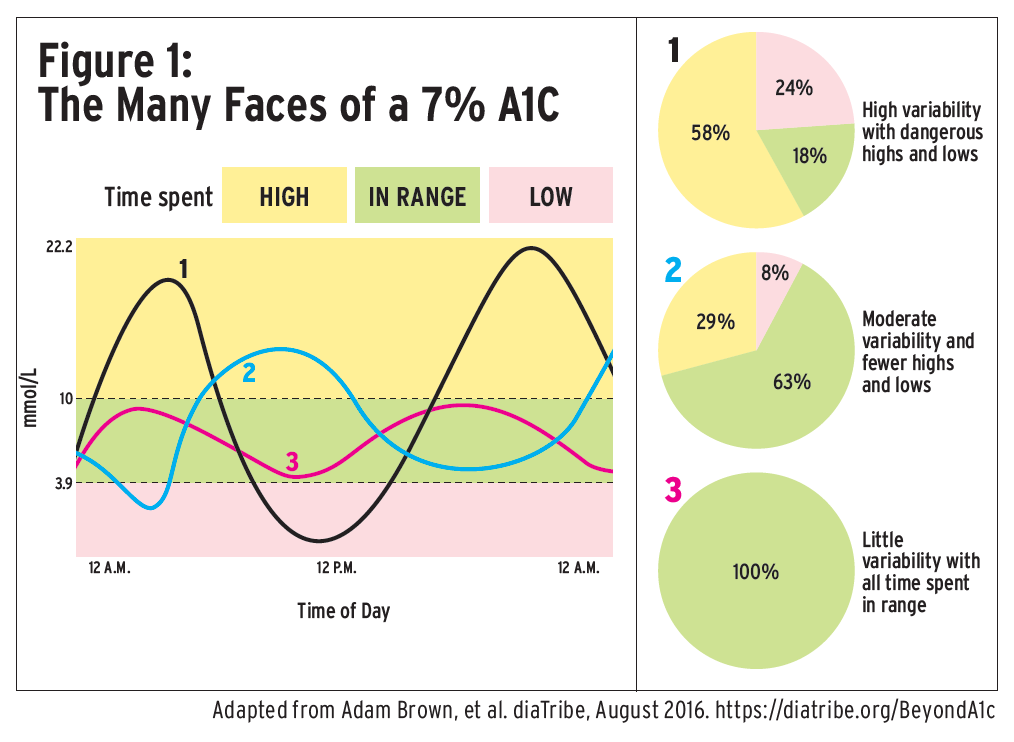
Instead of measuring average blood sugar via the A1C test, there is growing interest from diabetes experts in tracking time in range (TIR): the percentage of time that a person’s blood glucose level is in their recommended target range (see Glucose Targets). The A1C average does not capture glycemic variability, the fluctuations in glucose values of people living with diabetes. Two people can have the same A1C value but have a wide range of high and low blood glucose values, which results in a different TIR (see Figure 1).
A mean speed of 80 km/h over the past three months of commuting will never reflect times when a vehicle is racing at 150 km/h and far in excess of the speed limit or is slowed to 15 km/h in traffic congestion. Similarly, the clinician receives only the most basic of information from the HbA1c measurement and masks the occurrence and frequency of dangerous highs and lows.76
Time in range goals may be individualized for each person; however, generally people with diabetes should aim to be in-range as much as possible, with a recommendation of least 70% TIR. Evidence is growing that increased TIR reduces the likelihood of diabetes complications. Experts indicate that a TIR of 70% equates to an A1C of about 7%, and each 10% increase in TIR equates to a 0.5% decrease in A1C.
iii. Evidence-Based Guidance for Blood Glucose Monitoring
Diabetes Canada recently updated its blood glucose monitoring recommendations77, 78 for Canadians living with diabetes to reflect new and emerging research that has been conducted within the past few years. The recommendations on glucose monitoring type and frequency prioritize safety and improved outcomes for people living with diabetes. These recommendations offer healthcare providers evidence-based guidance on the types of devices that are best suited to people living with diabetes based on their disease type, medications and treatment goals.
Benefit plan managers may find it helpful to refer to these recommendations to determine coverage of glucose monitoring devices for employees or their family members living with diabetes.
iv. Benefits of Glucose Monitoring Devices79, 80, 81, 82, 83, 84, 85
According to Diabetes Canada, glucose monitoring devices such as intermittently scanned continuous glucose monitoring (isCGM) (formerly known as flash glucose monitoring) and real-time continuous glucose monitoring (rtCGM) (also known as continuous glucose monitoring or CGM) “have the potential to improve blood sugar management and quality of life for people living with diabetes, resulting in physical, social, emotional, and functional benefits.”86
Glucose monitoring technologies allow the person with diabetes to collect more data about their glucose, says Tanner, and “drive behaviour and lifestyle changes to improve their condition and make the day-to-day life with diabetes easier.”
Not only do the devices eliminate many of the finger pricks required by more traditional glucose
meters, but they also help people with diabetes stay within their target blood sugar range. Traditional blood glucose monitoring and A1C tests don’t capture glucose variability (the ups and downs of sugar levels) and don’t provide any indication of trends.
The devices may have alarms that alert people or their caregivers when their levels drop too low, for example, overnight while sleeping or while a child with diabetes is at school.
This can be particularly helpful for people with hypoglycemia unawareness.
Glucose monitoring devices can track and report glucose historical trend information, which allows the person with diabetes and their healthcare team to analyze glucose patterns and adapt treatment as needed. The devices allow remote tracking by healthcare providers to support digital diabetes care. In addition, real-time continuous glucose monitoring (rtCGM) can be integrated with insulin pumps to develop hybrid closed-loop insulin delivery systems (HCL), which automatically adjust insulin delivery based on rtCGM input.
Small Reduction Offers Significant Benefits
Reducing a person’s A1C by as little as 1% can lead to significant short and long-term clinical benefits.
Interventions or programs that reduce a person’s A1C by as little as 1% can lead to significant short- and long-term clinical benefits, including a 37% reduction in microvascular complications,87 43% reduction in amputations, 14% reduction in heart attacks and 12% reduction in strokes, and up to 21% reduction in deaths related to diabetes.88
v. Insulin Treatment89
Insulin therapy is required for the management of type 1 diabetes and sometimes type 2 diabetes. It is prescribed by healthcare providers based on people’s goals, lifestyle, meal plan, age and general health, as well as social and financial factors.
Insulin is injected by pen, syringe or insulin pump, and healthcare providers work with people with diabetes to determine the number, timing and dose of daily injections needed per day and whether an insulin pump is appropriate. The objective is to achieve blood glucose levels that are as close to target as possible to decrease hyperglycemia and avoid hypoglycemia.
v. Insulin Pumps90, 91,92,93
Insulin pumps94 are an alternative to multiple daily insulin injections, and their clinical effectiveness is well documented. Diabetes Canada’s Clinical Practice Guidelines state that insulin pump therapy can be beneficial for some people with type 1 diabetes.
Pumps can closely mimic the normal action of a healthy pancreas and allow glucose levels to be managed more precisely. They can be programmed to increase or decrease the amount of insulin delivered for a specified period or can calculate recommended insulin correction doses.
Insulin pumps can be life-changing for individuals living with type 1 diabetes, says Tanner. “Imagine having diabetes from a very young age, needing insulin injections four or more times per day. In one year alone, you would need a least 1,460 injections. An insulin pump takes away some of this burden.”
An insulin pump also allows flexibility with insulin delivery, explains Tanner. “A person can adjust their insulin depending on what they are doing and what they are eating, allowing them to match their insulin more precisely to their individual needs.”
Evidence shows that insulin pump users can achieve lower blood sugar levels, more time in range, less risk of hyperglycemia and hypoglycemia, and fewer associated long-term diabetes complications.
vii. Type 2 Diabetes Glucose-Lowering Medications95
As a complement to healthy behaviour interventions and lifestyle modifications, there are a variety of medications that may be used to treat type 2 diabetes that can help people achieve their target blood glucose levels. Diabetes Canada provides medication recommendations and encourages healthcare providers to work together with their patients to determine which medication(s) can help them achieve their best health.
|
First-line medication |
|
|
Metformin |
Makes the body respond better to insulin anduse it more effectively. Reduces liver’sglucose production. |
|
If metformin and healthy behaviour changes are not enough to manage blood glucose levels, second-line medications can be added. |
|
|
Second-line medications |
|
|
DPP-4 inhibitors |
Lower blood glucose by increasing insulin levels after meals and lowering glucagon levels (a hormone that raises blood glucose). |
|
GLP-1 receptor agonists |
Act when blood glucose increases after eating. Increase insulin levels, which helps lower blood glucose and lower glucagon levels (a hormone that raises blood glucose). |
|
SGLT2 inhibitors |
Eliminate glucose into the urine. |
|
Insulin secretagogues (meglitinides, sulfonylureas) |
Help the pancreas release more insulin. |
|
Thiazolidinediones |
Make the bodys tissues more sensitive to insulin. |
|
Insulin therapy |
Some people with type 2 diabetes need insulin therapy as well. Healthcare provider prescribe based on individual needs. |
Sponsored by:


44 http://guidelines.diabetes.ca/browse/chapter14#sec1
45 https://www.hqontario.ca/Portals/0/Documents/evidence/reports/hta-continuous-monitoring-of-glucose-for-type-1-diabetes-en.pdf
46 https://www.cdc.gov/diabetes/library/features/prevent- complications.html
47 https://www.mayoclinic.org/diseases-conditions/diabetes/in-depth/diabetes-management/art-20047963
48 https://www.cdc.gov/diabetes/library/features/prevent-complications.html
49 https://www.cdc.gov/diabetes/library/features/prevent- complications.html
50 https://www.diabetes.ca/managing-my-diabetes/tools---resources/abcdes-of-diabetes-care-quick-reference-guide
51 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Managing-My-Diabetes/Tools%20and%20Resources/my-diabetes-care-not-just about-blood-sugar.pdf?ext=.pdf
52 https://www.continuuminnovation.com/en/how-we-think/blog/understanding-the-whole-patient/
53 https://www.healthyplace.com/diabetes/mental-health/what-is-uncontrolled-diabetes
54 https://my.clevelandclinic.org/health/diseases/7104-diabetes- mellitus-an-overview
55 https://www.hopkinsmedicine.org/diabetes/diabetes_education/ patient_education_material/get_off_the_blood_glucose_ rollercoaster.pdf
56 http://www.diabetesincontrol.com/wp-content/uploads/2019/01/
42 FactorsPDFdiatribeCompressed.pdf
57 https://www.mayoclinic.org/diseases-conditions/diabetic-hypoglycemia/symptoms-causes/syc-20371525
58 https://guidelines.diabetes.ca/docs/patient-resources/lows-and-highs-blood-sugar-levels.pdf
59 https://specialfeature.diabetes.ca/2018/fear-of-hypoglycemia-doesnt-have-to-restrict-your-diabetes-management
60 https://www.diabetes.co.uk/hypo-unawareness.html
61 https://www.diabetesselfmanagement.com/diabetes-resources/definitions/hypoglycemia-unawareness/
62 https://www.hqontario.ca/Portals/0/Documents/evidence/reports/
hta-continuous-monitoring-of-glucose-for-type-1-diabetes-en.pdf
63 https://diatribe.org/detecting-signs-hyperglycemia-vs-hypoglycemia#Hyper
64 Sensing-based glucose monitoring technology such as flash glucose monitors and continuous glucose monitors do not measure blood glucose, but rather interstitial glucose levels, or the fluid that surrounds the cells of tissue below the skin.
65 https://www.diabetes.ca/managing-my-diabetes/tools---resources/managing-your-blood-sugar
66 https://www.canada.ca/en/public-health/services/chronic-diseases/reports-publications/diabetes/your-guide-diabetes.html
67 Also known as capillary blood glucose (CBG) test or self-monitored blood glucose (SMBG).
68 https://www.diabetes.ca/managing-my-diabetes/tools---resources/ managing-your-blood-sugar
69 https://www.canadianjournalofdiabetes.com/article/S1499- 2671(21)00195-7/fulltext
70 https://diatribe.org/time-range
71 https://diatribe.org/going-beyond-a1c-%E2%80%93-one-outcome-can%E2%80%99t-do-it-all
72 https://www.mysugr.com/en/blog/5-things-know-about-time-range/
73 https://pubmed.ncbi.nlm.nih.gov/30575414/
74 Battelino T, Danne T, Bergenstal RM, et al. Clinical Targets for Continuous Glucose Monitoring Data Interpretation: recommendations From the International Consensus on Time in Range. Diabetes Care 2019;42: 1593e603.
75 https://www.canadianjournalofdiabetes.com/article/S1499- 2671(21)00195-7/fulltext
76 Adapted from: https://www.liebertpub.com/doi/pdf/10.1089/ dia.2013.0060?download=true
77 https://www.canadianjournalofdiabetes.com/article/S1499- 2671(21)00195-7/fulltext
78 Diabetes Canada will soon be releasing this reimbursement policy statement.
79 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Managing- My Diabetes/Tools%20and%20Resources/Continuous_Glucose_Monitoring_Advocacy_Pkg_4.pdf?ext=.pdf
80 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Managing- My-Diabetes/Tools%20and%20Resources/Flash_Glucose_ Monitoring.pdf
81 https://waltzingthedragon.ca/diabetes/managing-bg/choosing-cgm-flash/
82 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Managing- My-Diabetes/Tools%20and%20Resources/Glucose_Monitoring_ Comparison_2.pdf
83 https://diabetes.ca/DiabetesCanadaWebsite/media/Advocacy-and- Policy/Advocacy%20Reports/Advanced_Glucose_Monitoring_EN_ OCT-2020.pdf
84 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Managing- My-Diabetes/Tools%20and%20Resources/Continuous_Glucose_ Monitoring_Advocacy_Pkg_4.pdf?ext=.pdf
85 https://diabetes.ca/DiabetesCanadaWebsite/media/Advocacy-and- Policy/Advocacy%20Reports/Advanced_Glucose_Monitoring_EN_ OCT-2020.pdf
86 https://diabetes.ca/DiabetesCanadaWebsite/media/Advocacy-and- Policy/Advocacy%20Reports/Advanced_Glucose_Monitoring_EN_ OCT-2020.pdf
87 Microvascular complications are those that affect small blood vessels such as retinopathy (vision loss or blindness), nephropathy (kidney damage) and neuropathy (nerve damage).
88 https://www.bmj.com/content/321/7258/405
89 http://guidelines.diabetes.ca/cpg/chapter12
90 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Advocacy-and-Policy/Advocacy%20Reports/Insulin-Pumps-Comparison-EN.pdf
91 https://waltzingthedragon.ca/diabetes/insulin-pumps-cgm/what-is-insulin-pump-how-does-it-work-parts/
92 https://www.aboutkidshealth.ca/Article?contentid=1733&language= English https://www.diabetes.co.uk/insulin-pumps/pros-cons-of-insulin-pumps.html
93 https://www.diabetes.ca/DiabetesCanadaWebsite/media/Advocacy-and-Policy/Advocacy%20Reports/Insulin-Pumps-Comparison-EN.pdf
94 Also referred to as continuous subcutaneous insulin infusion (CSII).
95 http://guidelines.diabetes.ca/cpg/chapter13
